Thought Leadership
On January 14, 2025, the FTC released its Second Interim Report, titled Specialty Generic Drugs: A Growing Profit Center for Vertically Integrated Pharmacy Benefit Managers.
Recent regulatory changes to the process state Medicaid pharmacy programs receive rebate payments from drug manufacturers are having significant implications for managed care pharmacy.
On February 5, 2024, a class action complaint was filed against one of the nation’s largest self-funded employers, Johnson & Johnson (J&J). In the case, Lewandoski v. Johnson & Johnson, the proposed class is claiming that J&J failed to uphold their fiduciary duty of prudence under ERISA.
HealthPlan Data Solutions (HDS) was selected by the leadership team of a state employee health plan representing nearly 300,000 covered lives to establish an industry leading pharmacy payment integrity program.
A mid-sized, regional health plan partnered with HealthPlan Data Solutions (HDS) to implement a differentiated pharmacy benefit oversight solution following years of poor experiences with their traditional PBM audit process.
As we begin another year, several major trends from 2023 will continue to drive key changes in the pharmacy benefit market for health plans and other plan sponsors. In this article, we detail three important trends worth following throughout 2024
A national health plan collaborated with HealthPlan Data Solutions (HDS) to initiate a pharmacy claim monitoring program. Implementing Claim Scan, the plan saved $12.3 million over two years.
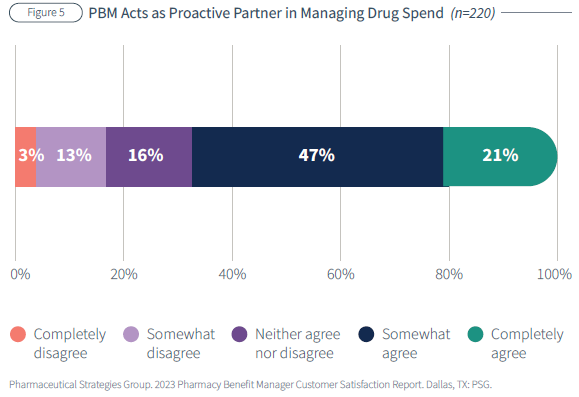
In 2023, the pharmacy benefit management (PBM) industry witnessed a significant shift in client sentiment. Health plans, employers, health systems and unions reported a notable decrease in satisfaction with their PBM vendors, as detailed in the 2023 Pharmacy Benefit Manager Customer Satisfaction Report by Pharmaceutical Strategies Group (PSG).
The Kraft Heinz Company is currently amid a $1.3 billion legal battle with one of their key healthcare vendors responsible for managing their medical benefit. More specifically, the lawsuit claims the medical benefit vendor “paid millions of dollars in provider claims that should have never been paid dating back to 2012.” While the case specifically pertains to the administration of the medical benefit, many parallels exist with the pharmacy benefit landscape at large.
In this article, HealthPlan Data Solutions’ (HDS) claims analysts will review the purpose and limitations of traditional PBM audits, offer insights to help health plans establish robust pharmacy payment integrity programs, and provide suggestions to enhance accountability in the pharmacy benefit.