Case Study
How HDS implemented Claim Scan real-time payment integrity to help one plan save $6.8M in the first year
At a Glance:
A mid-sized, regional health plan partnered with HealthPlan Data Solutions (HDS) to implement a differentiated pharmacy benefit oversight solution following years of poor experiences with their traditional PBM audit process. Frustrated by long audit resolution procedures, this health plan turned to HDS to implement Claim Scan, an ongoing pharmacy benefit monitoring program, for their 365,000 pharmacy lives across commercial, Medicare Advantage, and ACA lines of business.
Background & Situation
Prior to engaging with HDS to support their pharmacy benefit payment integrity efforts, this client mainly relied on traditional pharmacy benefit audits to ensure their PBM was performing appropriately to contract. While annual PBM audits serve as the cornerstone for many health plans to provide oversight to their pharmacy benefit, they are not a panacea and come with many limitations when used in isolation. These limitations soon became apparent to the client’s pharmacy team.
Starting in 2018, this client’s pharmacy team began voicing concerns about the significant time delays between their audits and actual monetary reconciliation efforts with their PBM. In one specific case, the lag between conducting their audit and delivery of preliminary findings took more than 18 months. By the time the findings were available to review, many of the claim discrepancies had become difficult to act on given turnover at both the client’s auditor and their PBM’s audit department. For one specific audit, the client’s pharmacy team noted that financial reconciliation wasn’t reached for almost 5-years and served as a continual headache for their team.
Frustrated with the level of engagement from their PBM, this client began looking for a partner to help them change tactics.

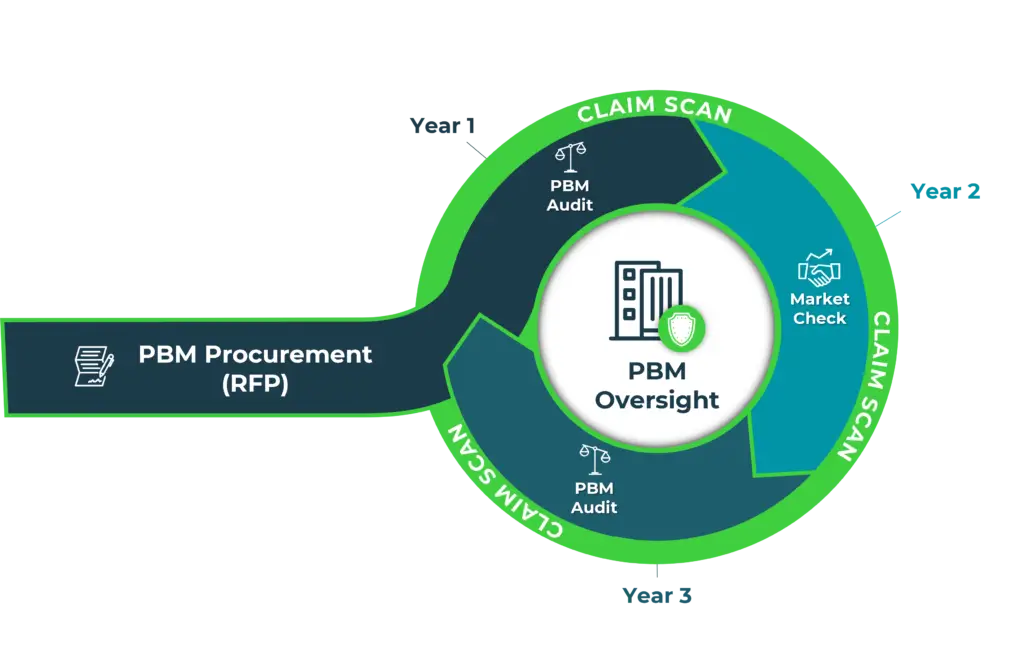
THE TRADITIONAL PBM OVERSIGHT MODEL WITH CLAIM SCAN
Solutions & Results
Ultimately, the client turned to HDS and their team of experienced pharmacy claims analysts to explore a new approach to driving healthcare affordability.
Together, HDS and the client implemented Claim Scan, an ongoing pharmacy benefit monitoring platform designed to ensure PBMs remain accountable to their contracts and highlight opportunities for savings. HDS worked directly with the client to map over 1,000 different plan design structures, PBM contracts, amendments, and more to review PBM adjudicated pharmacy claims at every invoice cycle throughout the plan year. Following implementation, HDS’s account management team conducted weekly meetings with the client’s pharmacy leadership team to review Claim Scan results and determine what findings to prioritize for resolution with the client’s PBM.

Through the implementation of Claim Scan, the client began to notice a dramatic difference in the depth and accountability of their payment integrity process. In the client’s first year with HDS, Claim Scan identified over $20 million in savings opportunities for review with the client’s PBM. From the initial list of findings, HDS was able to work together with the client and their PBM to secure $6.8 million dollars in realized savings. Claim Scan output was used to provide all the necessary data and contract language to drive financial resolution with the client’s PBM during the plan year.
The client noted that the level of detail the HDS clinical analytics team goes through with their pharmacy leaders during weekly status meetings was amazing. The client’s pharmacy leadership team believes one of the most valuable things about HDS is their ability to provide plans with all the data and power to drive for continuous improvement with their PBM and effectively drive out gray areas from their contracts.
Conclusion
Following their initial engagement with HealthPlan Data Solutions in 2022, this client has seen a dramatic improvement in their pharmacy benefit oversight efforts with the addition of Claim Scan ongoing monitoring. The client noted that they’re no longer at odds with their PBM about what their contract says and can focus on making sure the data and claims are adjudicating as expected. The ability to keep all parties fact based has led to improved relationships with the client’s PBM and allowed the client’s pharmacy team to feel positioned for continued success in controlling costs moving forward.
The main issues that pushed this client to search for an additive solution to their PBM auditing process are a thing of the past and have allowed the pharmacy team to do what they do best, improve member care.
