Commercial Payers
By combining hard data with human intelligence, HDS translates complex pharmacy benefit data into insight, enabling you to maximize the value of your PBM services, identify mid-contract opportunities for cost savings/avoidance, and ensure compliance. The HDS Spotlight platform brings payment integrity to the pharmacy benefit and offers services which are additive to existing PBM oversight and monitoring.
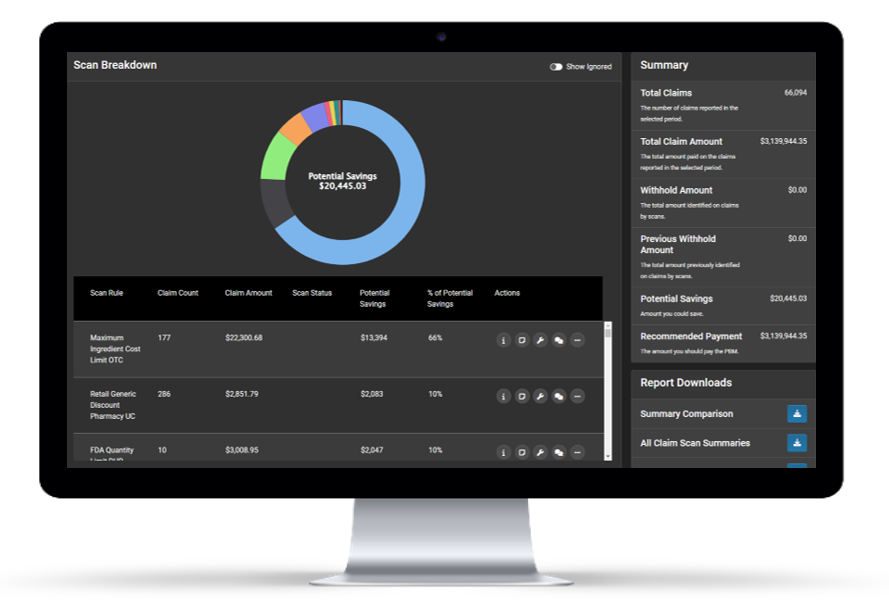
Providing Comprehensive Payment Integrity Through 100% Paid Claim Review
Identify
HDS proprietary pharmacy analytics technology identifies claim-level errors using 500+ scans in six key domains, including contract errors, plan design, and more.
Fix
Through our SaaS, hybrid, or fully outsourced model, perform comprehensive payment integrity and benefit oversight to resolve errors as they occur with the PBM.
Monitor
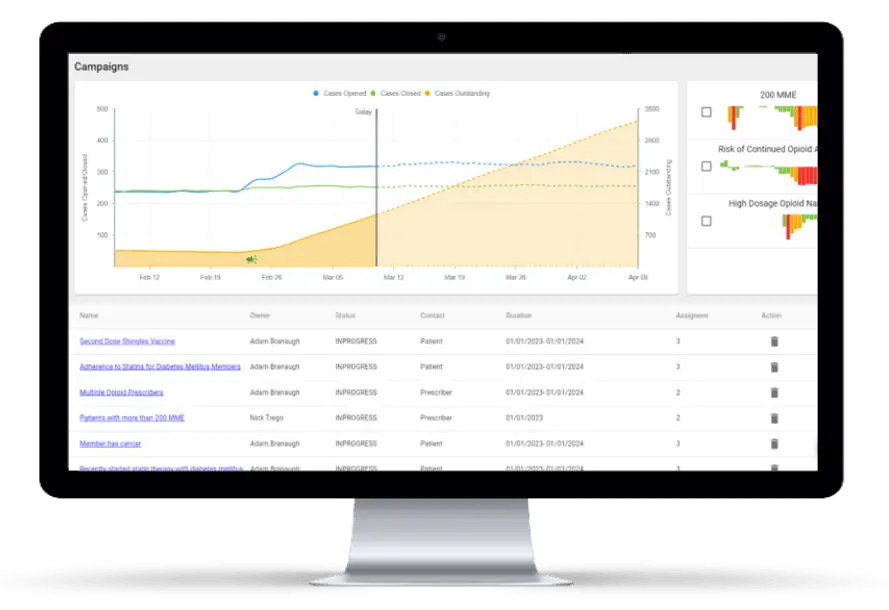
Once a fix has been implemented, the HDS platform continues to monitor the change over time to ensure its durability for the life of the contract.
Looking to Add Payment Integrity to Your Pharmacy Benefit?
Ensuring Payment Integrity for the Nation's Largest Commercial Payers
HDS is a software company that offers a holistic, post-adjudication, prepayment solution that cuts through contractual complexities and brings visibility and accuracy to your pharmacy spend data.
Commercial Plans
Commercial plans continue to see pharmacy costs increase 5% to 7% per year. HDS solutions and expertise not only identify erroneous adjudication and subsequent overspending, but help drive resolution, ensuring full transparency and appropriate payment for every claim.
Blue Cross Blue Shield Plans
Blues plans feel obligated to contract with a PBM owned by a competitor. HDS brings greater visibility to these transactional agreements to reduce spending and more efficiently manage plans. The HDS platform is PBM-agnostic, providing an enhanced layer of oversight to any PBM arrangement.