Government Payers
HDS is a software company that utilizes leading-edge technology and pharmacy expertise to analyze adjudicated prescription claims, monitor drug utilization trends, identify errors, and reclaim costs for all government payors, including Medicare, Medicaid, and Federal Employee Health Benefit Plans.
More Transparency. Better Engagement with Your PBM.
PBMs handle massive amounts of complex data, making it difficult to ensure appropriate payments are made in real time. HDS helps government payers work with PBMs to identify, fix, and monitor pharmacy claims errors, so they can demonstrate transparency and compliance with CMS standards, protect taxpayer funds, and improve health outcomes.
Identify
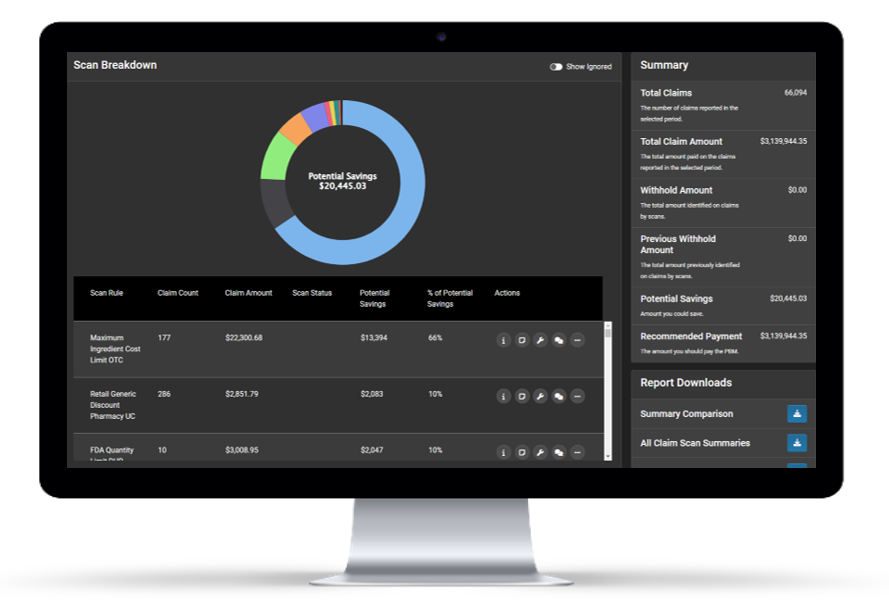
HDS proprietary pharmacy analytics technology identifies claim-level errors and using 250+ scans in five key domains, including contractual terms, plan design, and more.
Fix
Upon flagging a claim error, Federal and State health plans can work with their PBM vendor to quickly fix the issue and avoid unnecessary downstream costs.
Monitor
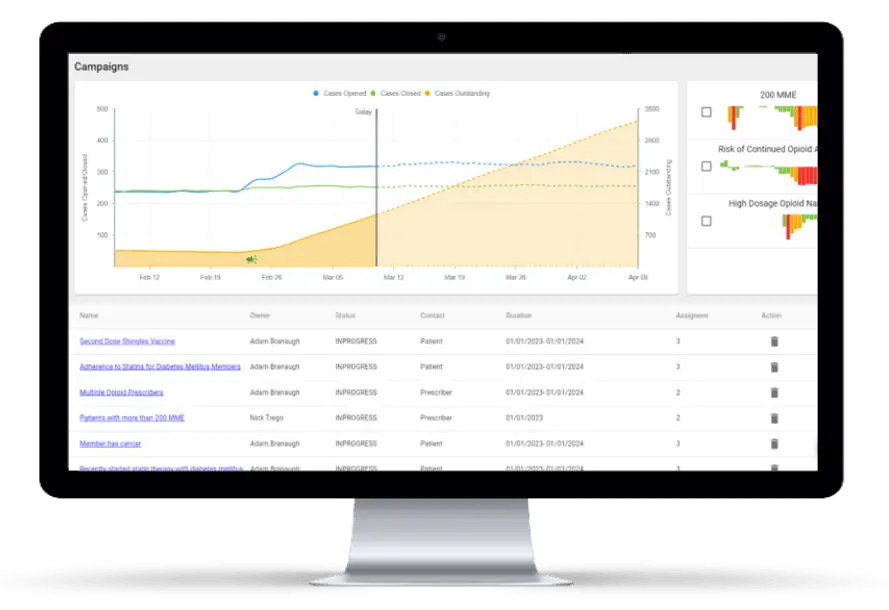
Once a fix has been implemented, the HDS platform continues to monitor the change over time to ensure its durability for the life of the contract.
Interested to See What Continuous Monitoring Would Look Like for Your Claims?
Ensuring Payment Integrity for Federal and State Health Plans
HDS offers a holistic, post-adjudication, pre-payment solution that cuts through contractual complexities and brings order and visibility to your pharmacy spend data.
Fee-for-Service and Managed Medicaid
HDS closely partners with states and Medicaid plans to ensure every claim is billed accurately, stretching their pharmacy dollars further while continuing to improve member health outcomes.
Medicare Advantage (MA) Plans
Aging populations, increased drug spend, and strict compliance requirements demand a stronger understanding of pharmacy spend. HDS enables the level of transparency needed to ensure optimal contract performance.
Federal Employee Health Benefit (FEHB) Plans
FEHB plans have distinct requirements and cost pressures. HDS is an expert steeped in experience and uniquely equipped to handle the challenges associated with FEHB plan oversight.