Solutions
Placing Comprehensive Pharmacy Benefit Management at Your Fingertips
HDS Spotlight delivers unparalleled pharmacy data analytics solutions to unlock the power of claims data and provide a single platform for continuous plan oversight, payment integrity, and cost savings.
HDS Spotlight delivers unparalleled pharmacy data analytics solutions to unlock the power of claims data and provide a single platform for continuous plan oversight, payment integrity, and cost savings.

Curb Pharmacy
Spend
Identifying ways to optimize pharmacy resources and reduce spend is critical. HDS solutions enable key stakeholders to slow the rate at which pharmacy spend is increasing through pharmacy data analytics and actionable insight.

Identify and Realize
Cost Savings
As opposed to retrospective solutions which limit intervention and recovery opportunities, HDS prospective solutions are used to identify savings opportunities as they occur. This allows for key stakeholders to make changes quickly to begin realizing savings and cost avoidance immediately.

Manage Benefit Oversight
in One Platform
HDS makes it easier than ever to illuminate your pharmacy benefit data through our single, web-based platform. HDS Spotlight and accompanying solutions bring comprehensive benefit management to your fingertips through a SaaS solution.
Pharmacy Data Insights
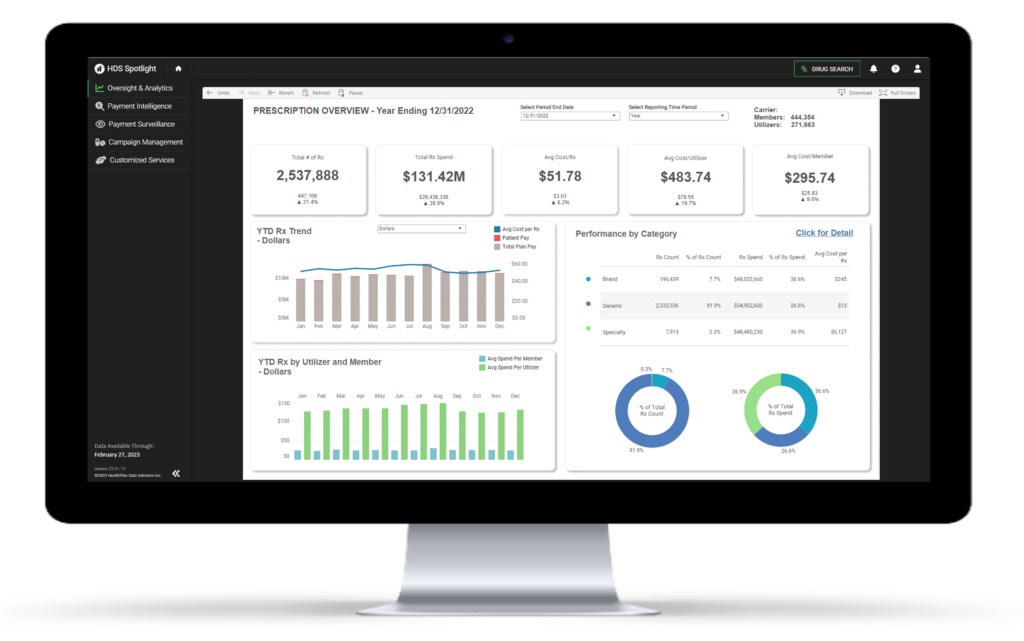
Rx Oversight & Analytics
One of the most powerful tools available to a pharmacy benefit stakeholder is their data. The HDS Rx Oversight & Analytics solution provides visibility and insight into pharmacy claim data through customized reporting, querying, dashboarding, and trending capabilities.
Payment Integrity
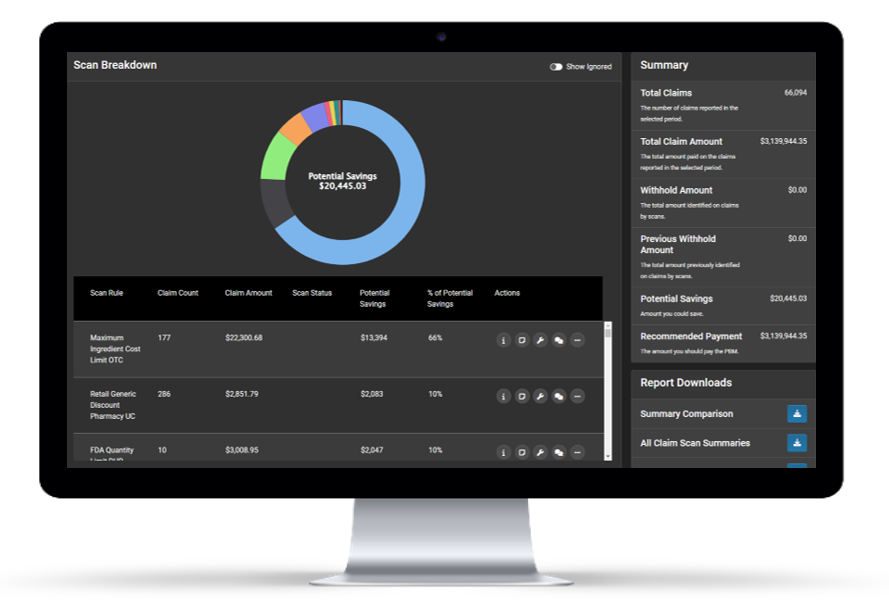
HDS Claim Scan
HDS is leading the way in payment intelligence using Claim Scan to turn identified claim errors into realized savings. Our SaaS-based platform empowers clients to monitor 100% of their pharmacy prescription claim data on a line item level to identify error as it occurs.
Campaign Management & Compliance
Campaign Management & Compliance
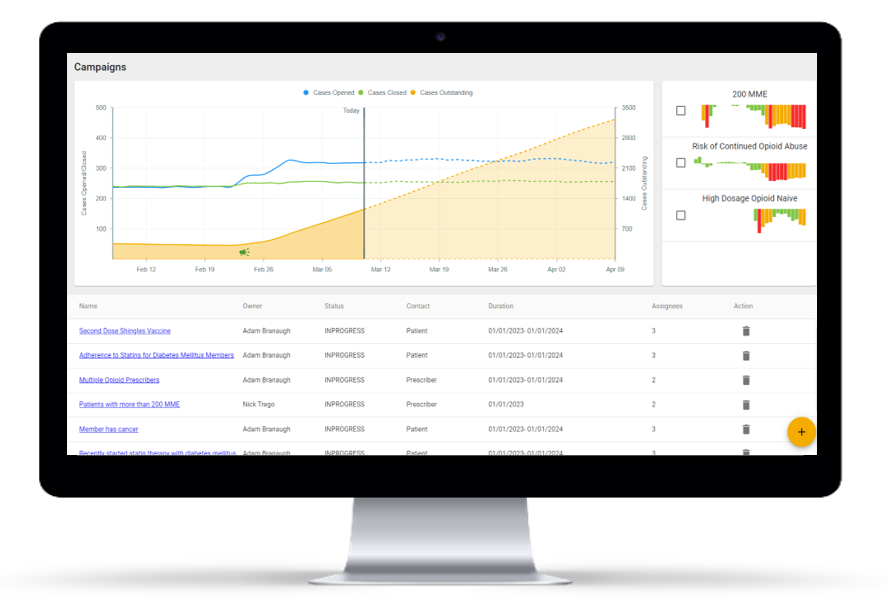
HDS RevealRx
Running successful member, provider, or pharmacy outreach campaigns can be critical to improving CMS STARS and HEDIS measures. Through using RevealRx, our clients can automate list creation, case tracking, and follow up to ensure outreach occurs for the right person with the right intervention at the right time.
Customized
Services
Audit | RFP | Contract Analysis
Pairing HDS Spotlight’s 100% claim review technology with our deep pharmacy benefit domain expertise enables our team to provide additive value to traditional pharmacy benefit services. Customized services offered by HDS include: Annual PBM Audits, PBM RFPs, and PBM Contract Analyses.