Payment Integrity
HDS Claim Scan
Ongoing Pharmacy Claim Monitoring
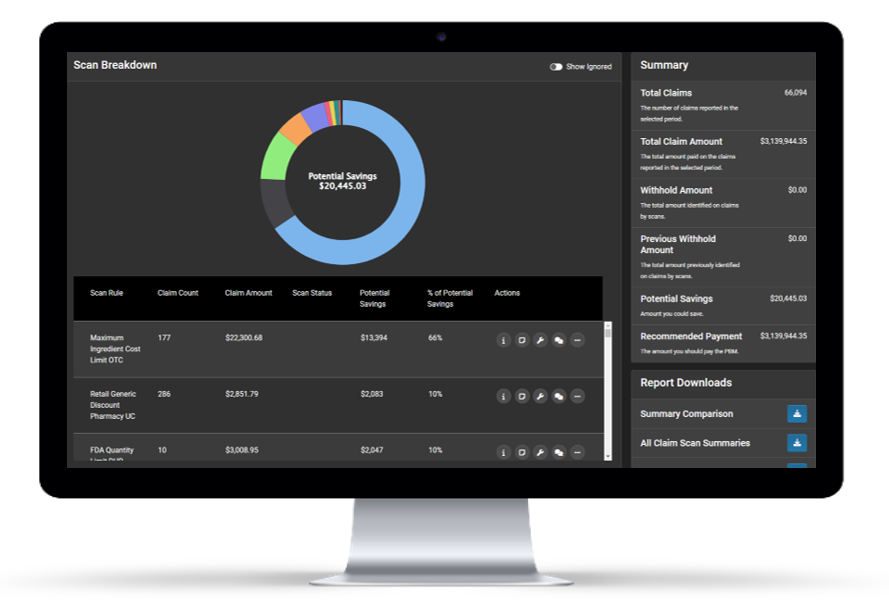
Claim Scan is a claims oversight solution which provides continuous analysis of 100% of prescription claims data. 400+ proprietary algorithms are deployed to analyze PBM performance against market competitive pricing, contract terms, plan design, regulatory requirements, and safety. Benefits of Claim Scan Include:
- Continuous and Ongoing Review of 100% of Pharmacy Claims
- Pre-Payment Integrity
- Self-Service (SaaS) or HDS-Service
- 400+ Proprietary Scans to Detect Claim Error
- Analyzes PBM performance against 5 key domains
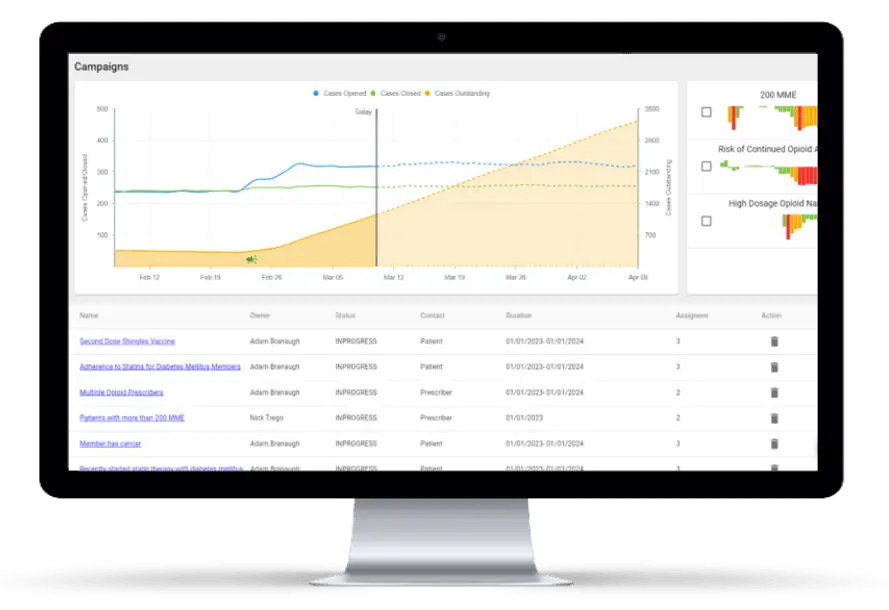
Platform Features:
Claim-Level Review
Full Visibility. Full Transparency.
The power of Claim Scan gives plan sponsors and other key stakeholders unfettered access to their data. As potential discrepancies arise, the platform allows users to view and investigate all impacted claims directly in the portal.
With information about the drug, fee, and pharmacy at your fingertips, researching impacted claims has never been easier. Once an error is validated, complete claims files can be exported with the click of a button and used in to inform the resolution process. Claim Scan makes pharmacy data actionable by providing a detailed analysis down to the claim level.
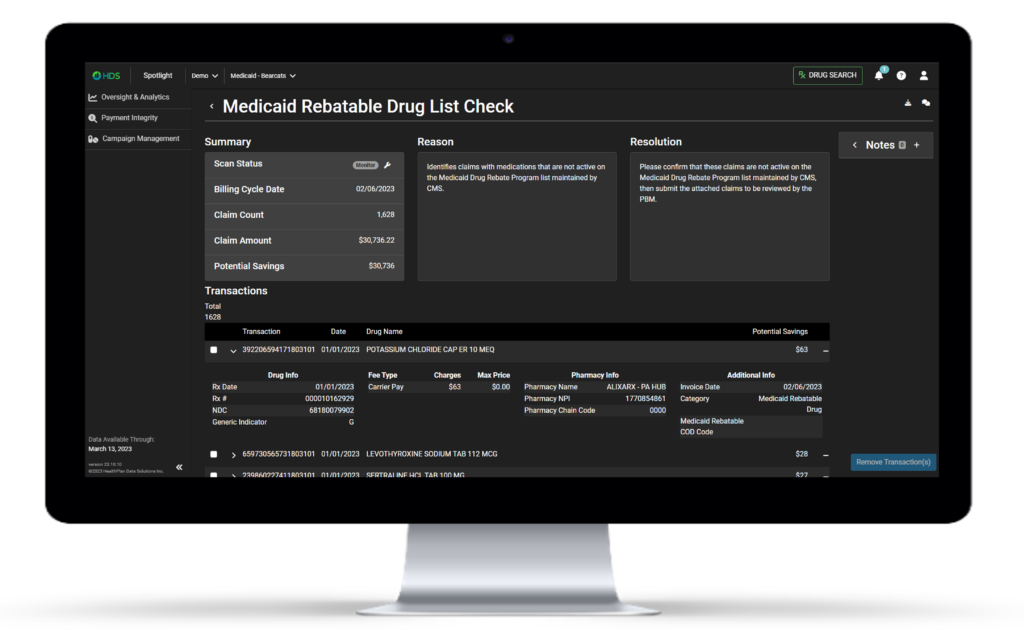
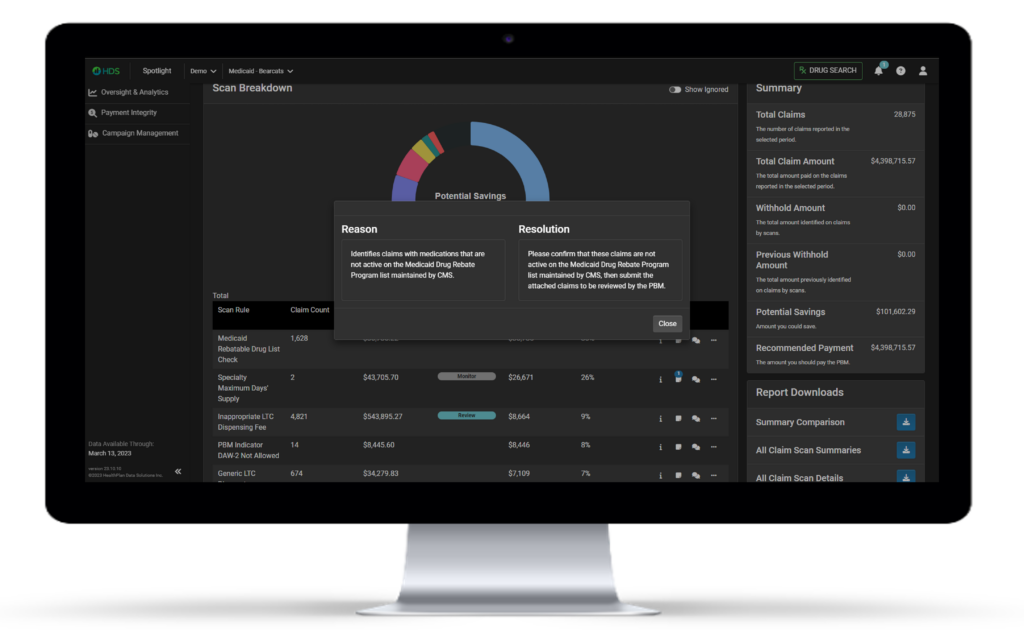
Scan Logic & Resolution
Step-by-Step Workflow to Maximize Recovery
With over a decade of experience in the pharmacy payment integrity space, our team has built a platform to not only identify errors, but effectively realize recoveries mid-plan year. In order to do this, claim findings must be accurate and resolution must be pursued differently based on the nature of the finding.
Our intuitive and data-rich dashboard allows stakeholders to manage all their pharmacy payment integrity efforts within a single platform. Each proprietary scan algorithm comes equipped with logic to help users quickly understand the nature of the finding. From there, users are provided with specific next steps to take with the PBM in order to realize recoveries from that error. Using our extensive experience, we help stakeholders pursue the appropriate pathways to maximize recovery.
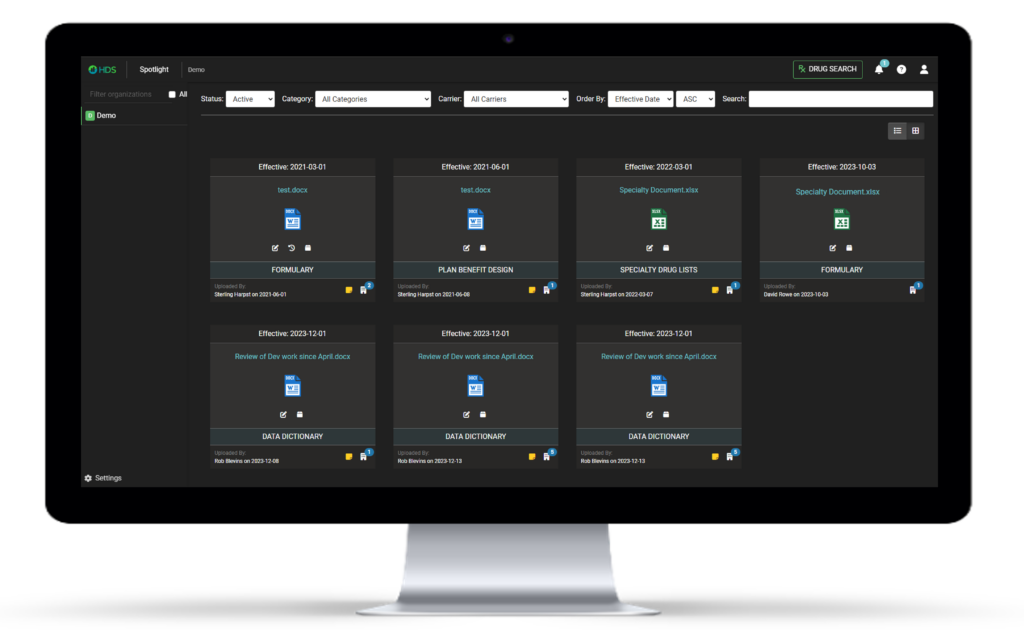
Document Repository
Easily Store & Access Critical Plan Documents
When it comes to managing your claim administration effectively, access to source of truth documents are essential. Unfortunately, most plans don’t have key documents such as plan designs, formularies, copay structures, or drug lists readily available.
Claim Scan solves this by providing a secure location to upload all documents pertaining to the plan. With the ability to filter, track revision history and take notes across the organization, the document repository makes it easy to manage all of your plan documents in one convenient location. Once files are uploaded, AI technology is able to read, interpret, and automatically update the logic for corresponding pharmacy claim algorithms.
How Does Ongoing Monitoring Compare to Traditional PBM Audits?